Medical Billing is a Process of Submission of Bills/Claims to the Insurance Company in a specified format for the service rendered (for the treatment given) by the doctor for the patient. Why the doctors approach the insurance company for the payment? Since the Majority of patients has insurance coverage and details of such coverage are provided to the doctor before the treatment. So it is the responsibility of the doctor to send the claims to the insurance company and get paid for the treatment given.
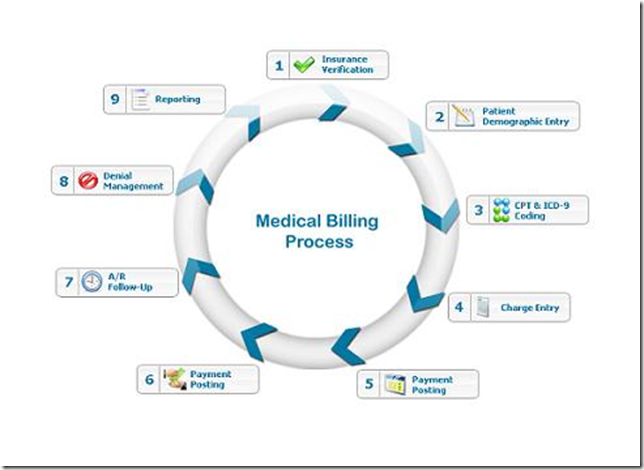
Here is the overall medical billing process. In the later section, we will see more detail on each section.
Insurance Verification:
Process started from here and usually front desk people are doing this process. Its a process of verifying the patients insurance is active or inactive by calling insurance or through online verification. If the insurance is inactive, it does not make any sense to send the claim/bill to the insurance company to get paid. So the front office people have to make sure that patient insurance is active even before the patient appointment. If the insurance is not active, then they have to collect the fee from the patient itself(In medical billing, this normally called as Self Pay claim or Patient Responsibility claim).
Charge Entry:
Charge entry is nothing preparing the claim to be sent to the insurance company. After getting the treatment details and patient disease details from the doctor, the billing department will start preparing the claim.The claim details, that are needed to get your insurance claims processed are entered here, and includes, the face sheet of the patient, doctor details, information about the insurance coverage of the patient and billing information.
Payment Posting:
Payment posting is simply posting payments from the insurance company into the system. The insurance company sends a check along with an Statement(This is statement is called as Explanation of benefit , shortly as EOB). On the EOB the insurance company will tell you the allowed amount and the amount they paid.
Denial Management:
The insurance companies reject(deny) paying claims for a number of reasons. Incomplete claim form, inconsistent patient information, etc.The insurance company indicates the reason for the denial in the Statement. Billing department will resolve those errors and again submit the claim to the insurance company.
Here is the overall medical billing process. In the later section, we will see more detail on each section.
Questions or feedback are always welcome. You can email me at vbsenthilinnet@gmail.com.

No comments:
Post a Comment